I Beat Cancer and All I Got Was This Lousy Personal Essay
Or, how I lost my pubes but kept my rectum in 2022.
8:21 AM CST on December 14, 2022
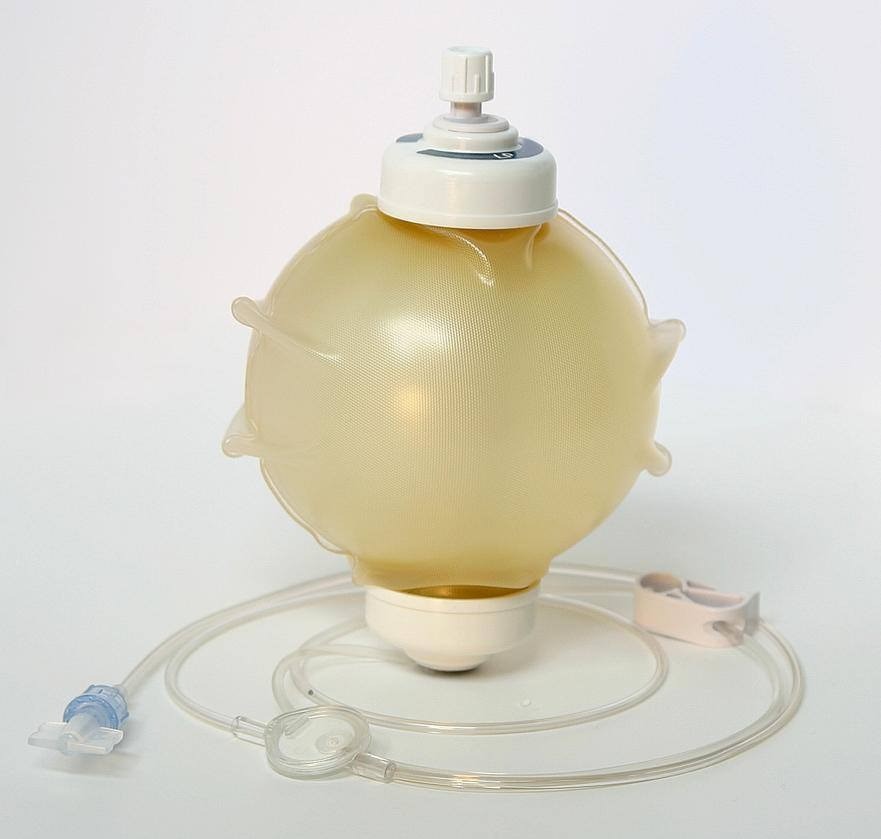
My chemo ball.
What’s even the point of getting cancer if you can’t write a deeply searching, emotionally resonant personal essay about it?
That question, admittedly trivial, vexed me in the later stages of my treatment for a rectal tumor a month ago. Chemo-related fatigue and drastically earlier sunsets combined to reduce my days to a string of naps occasionally broken by bouts of consciousness. This was not gripping medical drama.
Though never exactly a high-energy fellow, I was annoyed at my temporary lack of pep. But I was also peeved that, as I faced down my own mortality, I wasn’t having the life-changing crisis that both highbrow lit and schlock film had taught me to anticipate. Not that I expected to take up skydiving or find god or anything cliché like that, but aren’t serious illnesses supposed to alter your perspective on life in some significant way?
Yes, I had cancer. Cancer! CANCER! C-A-N-C-E-R!!! A word you dread saying out loud because it seems to confirm the worst. But as a catchall for cellular mutations of varying degrees of severity, from an easily excised melanoma to a metastatic storm wreaking havoc on your insides, the word can be misleading. The disease even behaves differently depending on where in the body it strikes.
My particular case, caught before spreading beyond my rectum, was hardly comparable to the more dire stories you’ve heard or maybe even lived through first- or secondhand. My cancer was serious, but not likely life-threatening—potentially curable via radiation and chemotherapy, and, if that failed, removable via surgery. I am technically “a survivor,” but compared to the experiences of folks who’ve endured much more painful and extensive treatment and beaten much worse odds, my own story feels so mundane that to join their club seems presumptuous.
There were no non-medical factors complicating my story either. I had adequate insurance, and enough money socked away to reach my out-of-pocket limit. I have thoughtful co-workers who were happy to let me take time off for appointments or recuperation. I had very little to worry about except my health.
And so without any real drama, without any pressing danger, where did that leave my dreams of a big personal essay? Wouldn’t I sound like just another old guy relating his ailments at a Denny’s? Aren’t our medical problems roughly as interesting to others as our dreams? Could I possibly snatch some meaning from this event? Or even just a couple reasonably engaging words? Read on to find out!
My first-ever colonoscopy back in March was routine, not long after I turned 52, and scheduled a couple years later than it should have been. (At the time, men were eligible for the procedure at 50; now that’s been altered to 45. Get that scope as soon as you can!) But it turned out to be quite an expedition for the surgeon, with all sorts of yet-benign growths needing to be hacked from my nethers. As he related the process afterward, I could practically see him in pith helmet, machete slashing a path through the overgrown wilds of my bowels.
I was so hopped up on whatever happy juice they sedated me with that when I awoke I barely noticed his reference to a lingering, unextractable growth in my rectum. But when I’d come down later that day, I thought, hmm, that sure doesn’t sound good. And then the biopsy results came back.
Now, a word about MyChart. The site, you may be aware, is a useful service some healthcare networks use that passes on messages from doctors and nurses, scheduled appointments, and test results. In the jumble of doctor’s visits and paperwork to come, it would prove incredibly convenient for me. Unfortunately, those test results are transmitted instantaneously to your inbox, before you’ve spoken with your doc. Which can make questionable test results an extreme source of anxiety if they come to your attention on, say, late Friday afternoon. Especially if, for instance, a biopsy says you have a rectal tumor.
And so began my weekend of existential uncertainty. My brain covered a lotta territory in those two days, let me tell you, all the way from “Well, that’s it—I’m gonna die” to “This is going to be so annoying.” Though I’d appreciate racking up a couple more decades first, I’m not personally afraid of being dead. I firmly believe it’s simply lights out, with no eternal encore of any sort. But dying? To waste away in increasing dependence was my worst fear, and even the more mundane aspects seemed daunting. Would I have to, as they say, “get my affairs in order”? What did that even mean, beyond clearing my laptop browser? And then there was the prospect—the necessity—of having to tell people I was dying. On top of everything else, preparing for death sounded like an incredible hassle.
I stewed in my own solitary visions of mortality that weekend. I live alone, so there was no one immediate to confide in, and as for reaching out to friends, what do you even tell anyone when you don’t know what’s happening to you? If you’re a person who dislikes breaking bad news to begin with (as I might just be) the prospect of sharing vague bad news is even less enticing. “Hi. I may or may not be dying. What’s new with you?”
I panicked so hard that weekend I think it made the rest of the year feel comparatively uneventful. But the tone of my doctor’s voice on Monday morning was reassuring. My tumor was serious but not likely deadly, though further scans were necessary. Which brings us to Keith’s Advice on Choosing an MRI Soundtrack. Once they put those headphones on, you’re stuck with your choice, and one three-minute song you happen to hate can feel like an eternity. Your best bet? Classic jazz. You’re almost guaranteed at least one cut from Kind of Blue, and the rest will be at least innocuous. Plus the clanging of the machine will create a modernist techno remix.
My MRI informed me that I had an “unremarkable pancreas” but also noted some irregularity with my thyroid and some nodules in my liver. This prolonged my anxiety at a slightly lower level for a short spell, till further tests classified the suspicious growths as a goiter and some ordinary fat deposits. I exhaled with relief.
And so began what I consider the fun part of my new life as a cancer patient. I learned that I can chat with oncologists for hours. Since communicating complicated diagnoses to patients is a big part of their job, they tend to be good talkers. And especially at a research hospital, if you show any interest in their thoughts, they are thrilled at the opportunity to nerd out and tell you what they know.
I was told that “the team” would discuss my case, which made me feel like a very special guest on House. And I was assigned to three oncologists, for surgery, radiation, and chemotherapy. Incidentally, I cannot say enough good things about the staff of M Health Fairview at the U of M Medical Center and Masonic Cancer Clinic. From the folks at check-in to the doctors, every person I dealt with was a pleasure. I was so impressed I even gave the radiation and chemo staffs thank you cards when I was done treatment, and I am not the sort of person who ever gets around to doing that.
My main source of conversation was my medical oncologist, Dr. Prakash, who was in charge of my chemotherapy regimen. My early questions were somewhat rudimentary. For instance: What is a rectum? As it was explained to me, it’s the tube between your colon and your anus that essentially regulates your bowel movements. When it’s time to go, it’s the rectum that sends the signal to your brain. Pretty useful.
Having covered the basics, we moved on to the specifics of my case. Determining the stage of my cancer was tricky, because my CT scan showed some enlarged lymph nodes. Was this metastasis from the tumor, or were they just inflamed or bruised by the cancer’s presence? Because of their placement, there was no way to figure out: The only way to take a sample without poking through the tumor itself, which would contaminate the biopsy.
Though I respected and got along well with my Fairview docs, I did what all good patients should and sought out a second opinion. And unfortunately, I got one. The folks at the Mayo Clinic evaluated me and came to the opposite conclusion. Don’t bother with treatment, they advised, just chop that pesky rectum out and get on with life. And so here I was, a non-expert having to decide between two expert opinions. I would have to go with my gut, which probably got me into this trouble in the first place.
I decided against immediate surgery. Though my rectum is hardly a part of my anatomy I feel a special sentimental attachment to, I’d rather not have my bowels scooped out like a Jack-o-Lantern. And recovery is a bit messy. They stitch your colon to your anus, and while that’s healing your wastes drips out of your small intestine into a colostomy bag. And while such apparatuses have become sleek and chic, I prefer shitting the old-fashioned way.
The roundabout route to possible recovery I chose was a two-step process. Part one was chemo-radiation. That meant 25 days of strolling past the ominous brutalist buildings near the medical center (I love ’em) to get zapped below the belt for 10 minutes or so, a process as painless as an X-ray. The first and last weeks were augmented by a daily regimen of chemo, pumped in through a port they’d inserted in my chest. After the radiation techs complained about my habitual lateness in the most Minnesotan way possible (“Is there another time that works better for you?”), I got my act together and we hit a nice rhythm. For a work-from-homer with an unstructured life, having a modest routine like this was a nice change of pace.
After a few weeks to let the radiation keep microwaving the tumor, it was time for real chemotherapy: five cycles, one every two weeks. I would bop across the river to the Masonic Cancer Center on 909 Fulton and get hooked up for a couple hours. (Again, the nurses were wonderful.) And when I left, I got to carry a little sack of poison home with me, about the size of a baseball, which was concealed in an over-the-shoulder pouch, allowing me to strut around with the world largely unaware that actual chemotherapy was happening but a few feet away from them. After two days, a nurse came to my house and detached the pump from my port.
As a cancer patient, I was a serious disappointment to my friends. They all naturally wanted to help, but there wasn’t much for them to do. I wasn’t incapacitated, so I didn’t need rides. I spent my three-hour cancer visits re-reading Robin Kelley’s excellent biography of Thelonious Monk, so I didn’t need company. I did generously allow them to bring me food, though, because I’m not too crazy about cooking even in happier moments. In my case, I think, having cancer turned out to be less taxing than knowing someone who had cancer.
My side effects were minimal. The plus side of getting cancer in your 50s, rather than in your 80s, is that your body has fewer ailments distracting it from the task at hand. By the end of my radiation treatment, I was experiencing what I can only call “rectal dry heaves,” if that tells you anything. Unpleasant, but like the worst of my chemo effects (mild mouth sores treatable with a salt water rinse) this only lasted a few days. I never experienced nausea, let alone vomiting; at worst, I felt a mild queasiness easily tamed with a quick pill.
My hair thinned a bit, which it might have eventually, and grayed a bit, which it surely would have eventually. The hair on my head, I mean—freakishly, my pubic hair fell out completely. One day I glanced down below my expanding gut (how did I gain weight during chemotherapy?) and the area below it was baby smooth. People apparently spend good money to achieve such a look.
The weirdest side-effect of all was a temporary neuropathy that made my skin extremely sensitive to cold. When I reached into the fridge, whatever I grabbed felt like a block of ice. My nose tingled at the slightest chill. And strangest of all, any drink below room temperature felt like it was crystalizing in my throat. Ice cream was out of the question. It was just the damnedest thing.
Sometime in October, I hit the wall, and the real fatigue settled in. A year of radiation and chemicals had caught up with me, and no matter how much I slept, I was never rested. Though I knew it was temporary, the loss of stamina bugged me. My Racket teammates were incredibly understanding, but still there were only four of us and the less I was available the more work they had to shoulder.
And then, one day in mid-November, my treatment was done.
Just last Thursday came The Scope of Truth, when I would learn if any malignant cells lingered in my bowels. This treatment was an all-or-nothing proposition. Either I was completely clear or it’d be on to the surgery I’d hoped to avoid.
Unlike a colonoscopy, which you pleasantly doze through, I was wide awake for this procedure, which was like having a plastic straw inserted through your asshole while you’re pumped up with air and water, or at least what I imagine that must feel like. But hey, at least I got to watch. (I wish I had pictures for you.) We were looking for a white scar, which proved so faint it took several passes. But then, there it was. My cancer was gone. All gone.
So, what does it feel like when a tumor that had no noticeable effect on your health no longer exists? It’s a strange, abstract sort of victory. You’ve prevented a danger you could easily have remained unaware of until it was too late. You’ve dodged a bullet you’ve never seen. I anticipated exhilaration, but felt only a sense of calm relief. Maybe I’d worried myself out early. Maybe it just hasn’t settled in yet, and sometime in the upcoming few years, which will be filled with regular scopes and scans to make sure the disease doesn’t come a-creeping back, my cancer-free life will seem as remarkable to me as it does to everyone I tell about it.
But maybe the lack of drama is my story. I was not afflicted with what a friend called “movie of the week cancer”—the stuff that devastates the body before it crushes it. Those are the stories we hear and tell, as we should, because they’re the most emotionally powerful and the stakes are at their highest. They’re what we have in mind when we hear the word “cancer.” But while I don’t have the precise numbers to back my assertion up, many people with cancer must experience the rather uneventful routine that I did.
The year only confirmed my belief that dark times aren’t necessarily our chief source of wisdom and growth, no matter what various religions and self-help regimens teach. When I think back on 2022, I’ll remember the chats I had with Dr. Prakash, the imperturbable kindness of the nurses in the oncology ward, my pride at relaying my doc’s comments to my brother and hearing him say “You’re really good at this.” (When it comes to learning on the fly and breaking complex matters down into understandable language, I suppose journalism teaches you some useful skills after all.) These small interactions added to my life far more than my white-knuckled weekend anticipating death ever did.
It’s too early to say how this experience will all affect me in the long term. With a new year on the horizon, will I come bursting back into the world after laying low for much of 2022?
Maybe. But for now, if you’ll excuse me, it’s time for a nap.
Stay in touch
Sign up for our free newsletter
More from Racket
It’s Your Very Last Complete Concert Calendar for April 2024: April 23-29
Pretty much all the live music you can catch in the Twin Cities this week.
THC Coffee: Not Your Friend’s Older Brother’s Wake ‘n’ Bake
THC cold brews from locals Venn Brewing and Gus Dean Coffee are all the buzz.
There Were Too Many People at the Waxahatchee Show!
This was not the ideal way to experience the mild turmoil of Katie Crutchfield's country-rock.
Everyone Is Being Super Normal About Isra Hirsi’s Arrest
Plus RIP Sammy McDowell, MN's new Supreme Court judges, and a Best Buy throwback in today's Flyover news roundup.
Ex-Guv/Aspiring Weed Tycoon Jesse Ventura Talks Timberwolves, THC, and Trump
The Navy SEAL/wrestler/actor/politician/conspiracy buff/businessman also reveals exactly how many speeches he has ever read off of a teleprompter.




